Arthroscopic meniscal surgery is one of the most frequently performed orthopedic interventions, particularly for athletes and highly active individuals. However, the most pressing question for patients post-surgery is: How long does it take to recover, and when can I return to normal activities?
The recovery trajectory is not uniform; it depends heavily on the surgical technique, individual healing biology, and adherence to postoperative rehabilitation protocols. To understand the timeline, one must first recognize the nature of the meniscal tear and its specific grade of severity.
Key Factors Determining Recovery Time
There are two core factors dictate the speed of recovery:
1. The Surgical Method Employed
This is the primary determinant of your timeline. There are two main arthroscopic approaches:
- Partial Meniscectomy: The surgeon debridates and removes the torn segment. Since no tissue healing is required, recovery is rapid, typically lasting 3 to 6 weeks.
- Meniscal Repair: The surgeon sutures the torn edges back together. Because the meniscus has a limited blood supply (especially in certain zones), the biological healing process is slow. Full recovery generally takes 3 to 6 months.
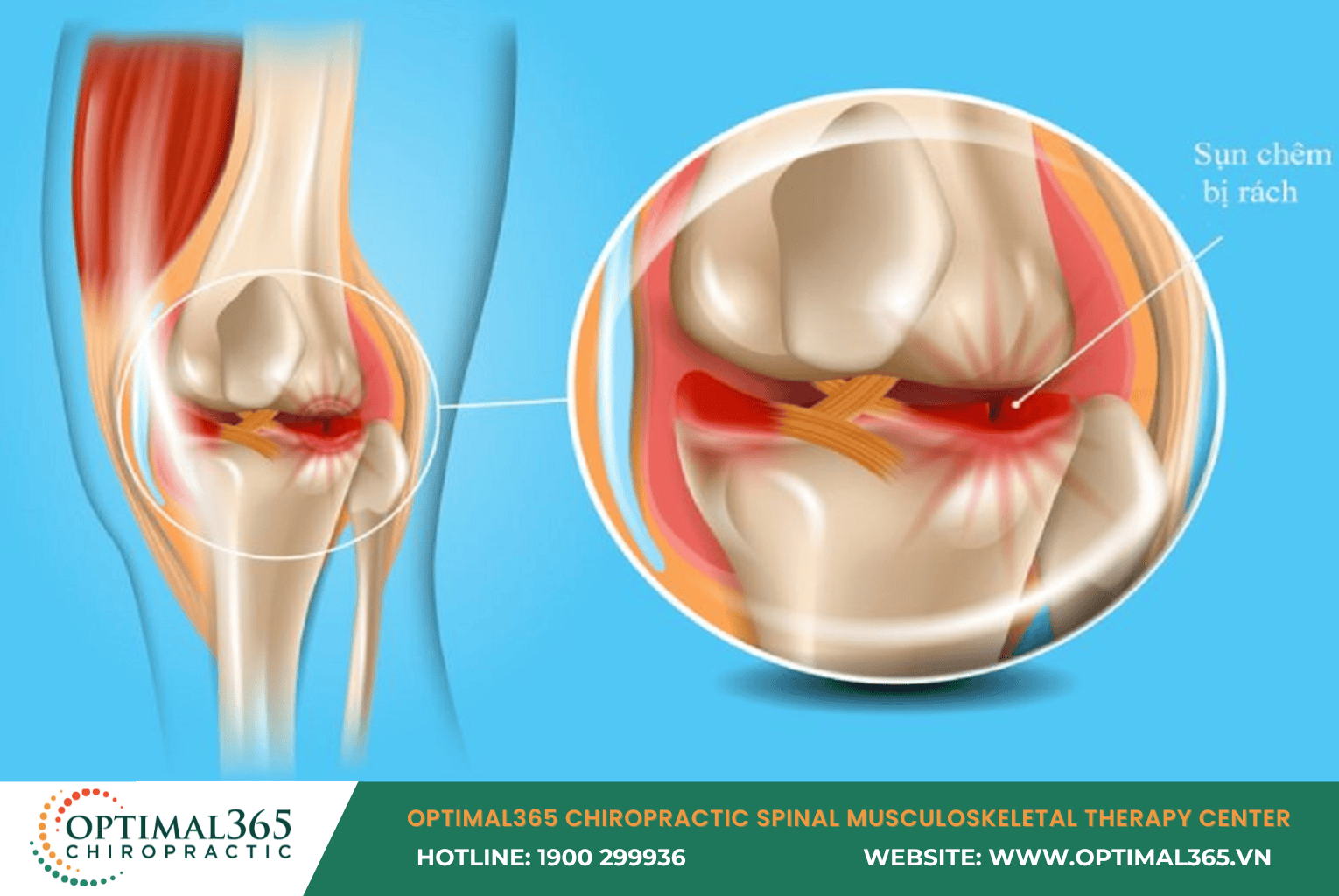
2. Tear Location and Morphology
The meniscus is divided into the “red zone” (vascularized) and the “white zone” (avascular). Tears in the red zone have a higher healing potential due to robust blood supply, significantly shortening the functional recovery period.
3. Concomitant Injuries
If the meniscal tear is associated with an Anterior Cruciate Ligament (ACL) rupture or chondral (cartilage) damage, the surgical complexity increases, and the recovery timeline can extend from 6 months to 1 year.
Post-Surgical Recovery Timeline: A Detailed 4-Stage Protocol
Below is the typical rehabilitation roadmap for a meniscal repair, which aims to preserve long-term joint function.
Phase 1: Weeks 0 – 2 (Protection and Edema Control)
The primary goal is to manage inflammation and protect the surgical site.
- Mobility: Patients typically use crutches with restricted weight-bearing (Non-Weight Bearing or Touch-Down Weight Bearing) as prescribed. A knee brace may be used for immobilization.
- Exercises: Focus on isometric quadriceps contractions to prevent muscle atrophy without stressing the repair.
- Management: Adherence to the RICE protocol (Rest, Ice, Compression, Elevation).
Phase 2: Weeks 2 – 6 (Restoring Range of Motion – ROM)
As the surgical incisions heal and swelling subsides, the focus shifts to joint mobility.
- Mobility: Gradual transition to Partial Weight Bearing (PWB). Crutches are discontinued once quadriceps strength is sufficient to stabilize the knee.
- Exercises: Progressive passive and active ROM exercises. Low-resistance stationary cycling may be introduced to promote joint lubrication.
Phase 3: Weeks 6 – 12 (Strength and Neuromuscular Control)
This is the “golden period” for restoring the musculoskeletal chain, specifically the quadriceps and hamstrings.
- Mobility: Normal gait patterns and slow stair climbing.
- Exercises: Shallow squats, proprioception (balance) training, and progressive resistance training.
- Precautions: Avoid deep squatting or sudden pivoting/torsional movements.
Phase 4: Month 3+ (Return to Functional Activity and Sport)
If functional tests are met, the patient can begin light jogging and sport-specific drills. However, returning to high-impact or contact sports usually requires 5 to 6 months of conditioning.
Postoperative Care to Accelerate Recovery
To optimize the healing window, patients must strictly adhere to the following:
- Mandatory Physical Therapy

Surgery addresses the mechanical defect, but physical therapy restores functional biomechanics. Neglecting rehab can lead to arthrofibrosis (joint stiffness) or re-tearing.
- Targeted Nutrition for Tissue Repair:
- Protein: Essential for myofibrillar repair.
- Vitamin C and Zinc: Critical for collagen synthesis and wound healing.
- Omega-3 Fatty Acids: Natural anti-inflammatory agents found in fatty fish.
- Calcium and Vitamin D: To maintain subchondral bone health.
- Weight Management: Excess body weight increases the mechanical load on the knee joint (roughly 4x the force of body weight during gait). Maintaining a healthy BMI is vital for protecting the repaired meniscus.
Red Flags: When to Contact Your Surgeon
Seek immediate medical attention if you experience:
- Sudden, localized swelling with erythema (redness) and heat.
- Purulent discharge or foul odor from the incision sites.
- Persistent high fever.
- Mechanical locking: The inability to fully extend the knee.
- Calf pain or swelling (potential signs of Deep Vein Thrombosis – DVT).
Comparison: Meniscectomy vs. Meniscal Repair
| Criterion | Partial Meniscectomy | Meniscal Repair |
| Crutch Use | 1 – 2 days (or none) | 2 – 6 weeks |
| Normal Gait | 1 – 2 weeks | 4 – 8 weeks |
| Driving | ~1 week | 4 – 6 weeks |
| Return to Sport | 4 – 8 weeks | 4 – 6 months |
| Degenerative Risk | Higher long-term risk of Osteoarthritis | Lower risk (Preserves joint cushion) |
Expert Perspective
Clinical data from the Cleveland Clinic emphasizes that the ultimate goal of meniscal surgery is not just immediate pain relief, but the prevention of early-onset Osteoarthritis. Experts at WebMD caution against premature weight-bearing, as overloading the repair site can lead to surgical failure. For athletes, specialists at Spire Knee highlight that patience during the first 3 months, combined with advanced biomechanical monitoring, is the key to extending the “lifespan” of the knee joint by 20–30 years.
Conclusion
Understanding the recovery timeline for a meniscal tear allows patients to prepare mentally and financially for the rehabilitation journey. Remember: the surgery is only the first step. Consistency in physical therapy and a disciplined lifestyle are what truly restore your mobility.
If you are experiencing chronic joint pain or stiffness, visit Optimal365 for a comprehensive musculoskeletal evaluation. Our team of experts will diagnose the root cause and provide an optimized recovery plan to help you return to your active lifestyle.